Summarizing the state of the climate, the month ended with extreme heat in the southern hemisphere where it’s summer, while high temperatures atypical of the northern hemisphere winter prevailed.
Parts of North and South America, northwest and southeast Africa, southeast and far eastern Asia, western Australia and Europe all saw record-breaking temperatures, either on a daily basis or for all of February.
“The anomalous heat is consistent with the persisting warming observed since June 2023, with seven consecutive new global monthly temperature records, including January 2024,” said Alvaro Silva, a climatologist working with WMO.
Global sea surface temperatures are record high. While the El Niño weather pattern “has stoked temperatures in some parts of the world, human induced climate change is the long-term major contributing factor,” he added.
Conversely, a large part of northwestern Canada, central Asia – and from southern central Siberia to southeastern China – witnessed exceptional cold during the last week of the month.
The meteorological winter in the northern hemisphere and summer in the southern hemisphere finish officially at the end of February.
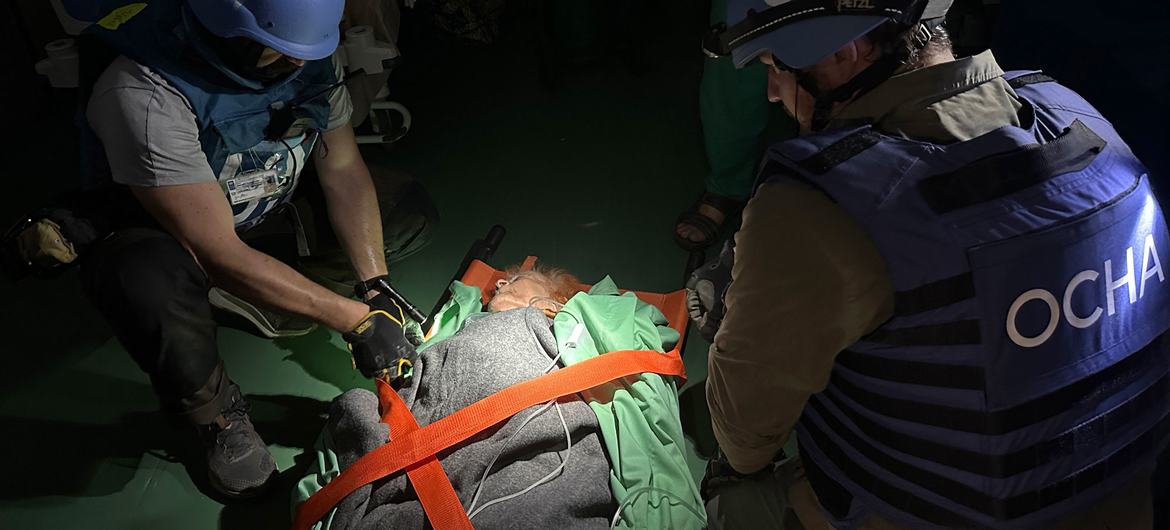
Sudanese continuing to flee into Chad: UN refugee agency
The UN refugee agency, UNHCR, raised increasing concern on Friday that more refugees will cross into Chad from Darfur in the coming weeks amid a worrying lack of food and other essentials.
UNHCRWestAfrica
Almost a year since the start of the civil war between rival militaries in Sudan, neighbouring Chad urgently needs more humanitarian aid and significant development investment, the agency reported, especially in its eastern areas which are hosting the refugee influx.
This investment will allow the country to continue its generous open-door stance towards refugees.
“Chadian officials are concerned that many more hungry Sudanese families will come in the next weeks,” said Kelly Clements, UNHCR’s Deputy High Commissioner, who is in the country to review the relief operation.
“The country is committed to keeping its borders open, despite the fragility of this region. But, doing so will put even more strain on Chad, which has so graciously been hosting refugees from Sudan’s war – now raging almost a year – and other refugees still here from earlier emergencies.”
State of emergency
In December, the World Food Programme (WFP) suspended rations to some refugee groups in the country due to lack of funds. Subsequently, the government declared a state of emergency for food and nutrition security.
Food distributions from Chad across the border to Darfur, where the security and protection situation is alarming, have not been made for well over a month, with cross-border aid recently suspended.
Women and children represent some 90 per cent of all refugees. Around 77 per cent of women arrived alone in Chad, with children.
Many have been exposed to gender-based violence including rape, said UNHCR, and now require comprehensive support. The agency provides medical and some psychological support, but much more is needed.
“Arrivals have slowed in the last months, but that could change quickly,” Ms. Clements said. “Even without more coming, needs now run well beyond the capacities of humanitarian agencies. There are very real fears that the border region faces another paltry lean season before heavy rains lash the camps.”
More than 553,150 new refugees from Sudan had been counted by mid-February, making the country the largest host of refugees fleeing Sudan since the brutal war between Government troops and RSF militia erupted in mid-April 2023.
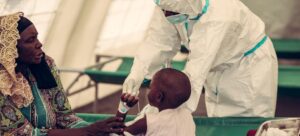
UNAIDS marks 10th anniversary of Zero Discrimination Day
Progress on advancing equality and fairness for all, regardless of gender, sexuality or HIV status, is in peril, said the UN agency dedicated to ending AIDS by 2030, marking Zero Discrimination Day.
The day of activism was established by UNAIDS a decade ago.
But, despite improvements in some societies, attacks on the rights of women and girls, of LGBTQ+ people and of other marginalized communities are increasing.
“The attacks on rights are a threat to freedom and democracy and are harmful to health. Stigma and discrimination obstruct HIV prevention, testing, treatment and care and hold back progress towards ending AIDS by 2030,” said Winnie Byanyima, Executive Director of UNAIDS. “It is only by protecting everyone’s rights that we can protect everyone’s health.”
At the start of the AIDS pandemic 40 years ago, two thirds of countries in the world criminalized LGBTQ+ people. Today, two thirds of countries do not, the agency noted.
Some 38 countries around the world have pledged to end HIV-related stigma and discrimination, and today, 50 million more girls are in school than in 2015.
UNAIDS said it was crucial to keep supporting women’s movements, LGBTQ+ rights as well as campaigns for racial justice, economic justice, climate justice and for an end to conflict.
The UN is by your side
“As communities across the world stand up for rights, the United Nations is not only on their side, but by their side,” said the agency in its statement marking the day.
On the day, and across the whole of March, events are being organised to remind the world of this vital lesson and call to action: by protecting everyone’s health, we can protect everyone’s rights.
“Through upholding rights for all, we will be able to achieve the Sustainable Development Goals (SDGs) and to secure a safer, fairer, kinder and happier world for everyone,” added Ms. Byanyima.